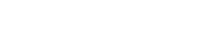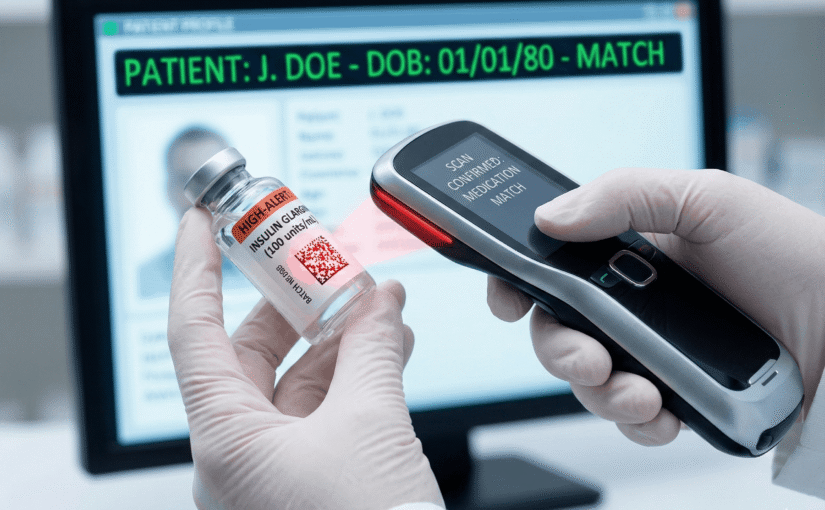
Manual transcription remains the single largest vector for clinical error in Australian pathology and pharmacy workflows.
When a clinician relies on handwriting or manual data entry to track specimens, the probability of a “never event” increases significantly. Hospital procurement managers and nurse unit managers understand that the cost of a mislabelled sample extends far beyond the financial burden of re-testing. It compromises patient safety and erodes trust in the healthcare facility.
Integrating robust barcode labelling systems is no longer a luxury for high-volume laboratories; it is a fundamental requirement for risk management. The shift from analogue identification to digital scanning removes the variable of human fatigue from the equation.
While many facilities have adopted basic scanning, the next tier of compliance involves end-to-end tracking that integrates seamlessly with Laboratory Information Systems (LIS) and Hospital Information Systems (HIS). Mermed engineers solutions that bridge the gap between physical inventory and digital records because we recognise that precision is the only acceptable standard in healthcare.
Quantifying the impact of automating identification
The argument for automation often centres on speed, yet the primary dividend is safety. A pivotal study published in Frontiers in Medicine analysed the impact of barcode-based tracking on pre-analytical errors. The data revealed that barcoding reduced laboratory testing errors from 2.26 to just 0.17 per 10,000 specimens. This drastic reduction illustrates how technology acts as a rigid firewall against the cognitive slips that occur during high-pressure shifts.
This level of precision is critical when managing high-alert medications or irreplaceable biopsy samples. The Australian Commission on Safety and Quality in Health Care (ACSQHC) reports that medication errors remain a significant cause of hospital admissions and adverse events. By implementing point-of-care barcode scanning, pharmacies effectively force a digital “hard stop” if a medication does not match the patient’s electronic profile. This workflow allows pharmacists and technicians to focus on clinical validation rather than rote verification.
Implementing these systems requires more than purchasing a scanner. It demands an audit of the physical environment where labelling occurs. Labels must withstand cryogenic freezing, autoclave sterilisation, and chemical exposure without degrading. A barcode that becomes unreadable due to moisture or abrasion renders the entire tracking system useless.
Meeting NSQHS standards through digital precision
Australian healthcare facilities operate under the strict governance of the National Safety and Quality Health Service (NSQHS) Standards. Standard 6 specifically addresses Communicating for Safety, with a heavy emphasis on correct patient identification and procedure matching. Manual checks are inherently fallible because they rely on the “two-person check” methodology, which is susceptible to confirmation bias.
Barcode labelling systems support accreditation by creating an immutable digital audit trail. When a nurse scans a patient’s wristband and the corresponding medication label, the system logs the interaction with a timestamp and user ID. This automated documentation proves invaluable during accreditation audits. It demonstrates that the facility does not merely have a policy for patient safety but employs engineered controls to enforce it.
Clinical leaders co-design these workflows to ensure they do not add friction to clinical care. A well-designed system functions in the background. It should empower practitioners to work faster while maintaining stricter compliance guardrails. When the scanner beeps, it provides immediate confirmation that the chain of custody is intact.
Optimising inventory control and supply chain security
Beyond patient safety, barcode technology stabilises the often volatile supply chain within hospital pharmacies and pathology centres. Stockouts of critical reagents or medications disrupt patient care and force procurement teams into reactive, expensive purchasing cycles. Manual inventory counts are time-consuming and prone to counting errors that skew data.
Automated inventory tracking creates real-time visibility. As items are scanned upon receipt and again upon dispensation, the central system updates stock levels instantly. This data allows for predictive modelling. Procurement managers can identify usage trends and adjust par levels before a shortage occurs.
GS1 Australia highlights that standardised barcoding across the supply chain improves traceability for recalls. If a specific batch of reagent is flagged for a quality issue, a robust system allows the laboratory manager to instantly locate every affected unit. This capability transforms a potential crisis into a manageable administrative task. It protects the facility from using compromised stock and ensures continuity of care.
Engineering a fail-safe workflow
Adopting this technology requires a partnership between clinical staff, IT departments, and solution providers. The hardware must suit the physical constraints of the workspace, and the consumables must match the specific rigours of the environment. Mermed supports this transition by supplying locally engineered labelling solutions designed specifically for Australian medical contexts.
Key considerations for a robust system include:
- Substrate Durability: Labels for pathology must survive liquid nitrogen storage and tissue processing chemicals.
- Adhesive Performance: Labels must adhere securely to curved surfaces like vials and test tubes without flagging or peeling.
- Print Clarity: High-resolution thermal printing ensures 2D barcodes remain scannable even at small sizes.
- Integration: The middleware must communicate flawlessly with existing patient administration systems to prevent data silos.
We encourage procurement and nurse unit managers to view labelling not as a consumable cost but as a component of their safety infrastructure. The investment in high-quality, validated labels and scanning hardware pays for itself by preventing the catastrophic costs associated with clinical error.
Barcode labelling reduces clinic error rates
The transition to fully automated barcode labelling systems is a critical step in modernising Australian pathology and pharmacy operations. The evidence is clear. Dropping error rates from over two per 10,000 to nearly zero represents a profound improvement in patient safety.
By aligning with NSQHS standards and leveraging technology to secure the supply chain, healthcare providers protect their patients and their practitioners. Precision creates safety, and in our field, safety is everything.